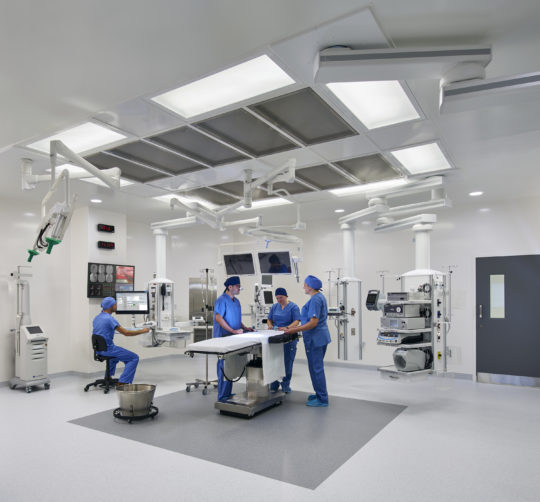
Lighting in healthcare centres requires balance between aesthetics and functionality. The right illumination is essential for medical staff to perform their duties and, as growing consensus suggests, aid in patients’ recovery. Bradford Keen speaks to architects and lighting specialists working across three continents about light’s healing properties.
From ancient Egyptians worshiping the sun god Ra to a parent parting the bedroom curtains of a moping teenager, light intuitively feels right. It is able to create perspective and alter moods. When intuition is verified by science, we feel vindicated by our innate wisdom.
Light has long been manipulated in effective design, but it is now permeating healthcare centres too. Gone are the days of bright, blue lights bearing down from above with the promise of sterility. Instead, the shifting ethos, backed by medical studies, has evolved to focus on how natural and artificial light can give patients a healthy glow.
“About five to ten years ago, healthcare design had a lot more of a clinical and institutional feel,” says Philip Schuyler. “People used really high colour temperatures – over 4,000k.” The electrical engineer at HH Angus explains that the industry now seeks to create a soothing environment mimicking someone’s home or a communal space, while balancing aesthetics, cost efficiency and functionality.
HH Angus and CanonDesign have undertaken a mammoth project. Spanning two blocks in downtown Montreal, the 21-storey Centre Hospitalier de l’Université de Montréal (CHUM) subsumes three existing facilities – Hôtel Dieu, Hôpital St Luc and Hôpital Notre-Dame – in what will be one of North America’s largest academic medical centres, spanning three million square feet. Phase one of the project, which includes the hospital and ambulatory building, was completed recently, while phase two’s office building is set for 2021. The healthcare district is set to teem with social activity, boasting an amphitheatre,
natural green spaces and one of the country’s largest displays of artwork.
The direct health benefits of lighting – improved mood, reduced hospital stay, lower mortality rates, among others – are proven, as is light’s ability to help create a sense of shared calm for patients and their loved ones.
“Lighting makes people feel a lot more receptive to treatment,” Jocelyn Stroupe, director of healthcare interiors at CanonDesign, says. “Often, healthcare encounters are filled with anxiety. We want to be sure anyone who enters the building feels a sense of comfort.”
This mindset of making hospitals communal and homely spaces is relatively new but gaining credence among architects.
“People usually go into healthcare facilities with humility,” says architect Joaquin Perez-Goicoechea. “They are searching for something; they need support and, if the building can help them achieve this, it brings satisfaction to all of us.”
This was the weighted starting point for the cofounder of AGi architects when designing the Hisham Al Alsager Cardiac Center in Kuwait. “People with chronic diseases require constant contact with doctors,” says Perez- Goicoechea. Their loved ones often spend many hours at their side or in the facility, which motivated the architect to design the centre as a place for social cohesion. “Light is extremely important for this. It must be a sanctuary,” he adds.
With red aluminium panels, the cardiac centre is designed and coloured – at the behest of the medical staff – to resemble a heart. Its large windows, on the north facade, open up to the dazzling blue of Kuwait Bay.
The multiple vertical skylights maximise natural light. Pollution and dust dictated their positioning. Placed flat and horizontally, they would have gathered too much grime, rendering them useless even with a stringent maintenance plan.
Lighting is a powerful “abstract and immaterial architectural tool,” says Perez-Goicoechea. “The issue is how you see the space as a structure on a sequence, which is identified by different lighting experiences depending on the use or character you want to give to that space.
“If you are going to be sitting in a waiting area for half a day, because this is the reality, you don’t want to be sitting under white, fluorescent lights. You want to be under warm ambient lighting that makes it cosier; it frames the space.”